Introduction
Elevated intraocular pressure (IOP) has long been considered the primary cause of glaucoma. Disease causing factors unrelated to IOP have also been linked to glaucoma.
Recently, many studies have emphasized the role of altered ocular blood flow and intermittent components of the pathway to glaucoma, such as vasospasm, free radicals, calcium influx to ischemic axons, calcium stimulated destructive enzymes, apoptosis and loss of nerve growth factors may all play a significant role in the disease. Specific vascular risk factors include vasospastic events that impair autoregulation, hemodynamic changes that reduce perfusion pressure, e.g., hypotension, organic changes in vessel walls and hematological disturbances such as increased blood viscosity that increases local vascular resistance and decreases perfusion pressure. These vascular factors can play a role in the pathogenesis of glaucomatous damage through reduced blood flow to the optic nerve head.
Anatomy
 The ophthalmic artery is the first major branch of the internal carotid artery.
It crosses the optic nerve and branches in a variable pattern. Two separate vascular systems are involved in
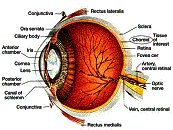
the nutrition of the posterior segment: the retinal vessels and the ciliary vessels. The central retinal artery enters the optic nerve about 10mm behind the eyeball. At the disc it branches into 4 major
vessels forming the vascular network of the inner layers of the retina and supplies the superficial part of the nerve fiber layer of the optic nerve head. Two posterior ciliary arteries originate from the ophthalmic artery. Each divides into 10-20 branches which penetrate the sclera at the posterior pole to form the choroidal capillaries, a dense one layer network.
The ophthalmic artery is the first major branch of the internal carotid artery.
It crosses the optic nerve and branches in a variable pattern. Two separate vascular systems are involved in
the nutrition of the posterior segment: the retinal vessels and the ciliary vessels. The central retinal artery enters the optic nerve about 10mm behind the eyeball. At the disc it branches into 4 major
vessels forming the vascular network of the inner layers of the retina and supplies the superficial part of the nerve fiber layer of the optic nerve head. Two posterior ciliary arteries originate from the ophthalmic artery. Each divides into 10-20 branches which penetrate the sclera at the posterior pole to form the choroidal capillaries, a dense one layer network.
Physiology
The retina and optic nerve head are autoregulated. This is achieved by regulating the vascular tone of resistant vessels. The vascular tone depends on the contractile state of smooth muscle cells and pericytes. These in turn are regulated by neurotransmitters, circulating hormones, myogenic and local metabolic factors as well as by endothelium derived factors. Endothelial released moderaters include nitric oxide and prostacyclin which are potent vasodilators. Endothelin and angiotensin are vasoconstrictors. Through the secretion of these vasoactive substances, endothelial cells can profoundly modulate local vascular tone.
A dysfunction, e.g., vasospasm, of the complex local regulatory systems may lead to hypoperfusion. A breakdown in the autoregulation of the optic nerve head has been proposed as a mechanism in glaucomatous damage. In glaucoma, vascular tone is disturbed because responses to endogenous relaxing factors are blunted or vessels respond more readily to vasoconstriction. It has been shown that patients with normal tension glaucoma have higher plasma levels of the vasoconstrictor endothelin-1, when compared with patients with open angle glaucoma. Others have shown an increased postural sensitivity to endothelin in patients with normal tension glaucoma. Calcium channel blockers inhibit endothelin-1 induced vasoconstriction and play a role in treatment of vasospasm related glaucoma.
Clinical Studies
Clinical studies have demonstrated that the microcirculation is disturbed in glaucoma. Reduced ocular blood flow velocity may contribute to glaucomatous damage. A variety of clinical studies have shown an association between systemic vascular conditions such as hypertension, diabetes, migraine, vasospastic peripheral disease and glaucoma. Glaucomatous damage appears to develop at a lower IOP in patients with diabetes reflecting reduced capillary blood flow at the optic nerve head. Certain vitamins, minerals, antioxidants, phytochemicals and other nutrients have been shown to be necessary for proper hemodynamics and overall health of the vasculature in the eye.
Future research will provide more answers to the role of vascular insufficiency in glaucoma and the importance of key nutrients to ocular health and will provide a more substantiated approach to the use of vasoactive medications and
supplements in targeted patients.
Nutrients and Ocular Blood Flow
Improving blood flow to the microvasculature and ensuring delivery of key nutrients to the eye may help keep ocular tissues healthy.
 |
Magnesium, when metabolized by the body and available at the cellular level, acts as a physiological calcium channel blocker and helps control important ocular vascular modulators. Calcium channel blockers have been reported to improve both ocular blood flow and visual function. In addition, magnesium reduces the production of endothelin-1, a potent vasoconstrictor, by the vascular endothelium. Magnesium
deficiency has been tied to increased intraocular pressure, vasospasm/vasoconstriction, restricted blood flow to the eye and primary open angle glaucoma. |
Antioxidants, B complex vitamins including folic acid and gingko biloba have also been shown to provide additional benefits to the microvasculature of eyecare patients.
|

