 |
|
|
Osteoporosis/Bone
Health
|
|
|
What is Osteoporosis?
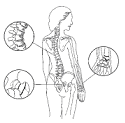
The term osteoporosis literally means “porous bones” (see figure 1). Osteoporosis is characterized by low bone mass and structural deterioration of bone tissue, leading to bone fragility and an increased susceptibility to fractures. Bones are living tissues that are constantly being lost and reformed. When bone loss is greater than bone formation, osteoporosis occurs. Osteoporosis is often referred to as the “silent thief” – bone loss progressing painlessly without symptoms until a fracture occurs. People may not know that they have osteoporosis until their bones become so weak that a sudden strain, a minor bump, or a low impact fall causes a fracture.
|
|
 |
|
Normal Bone
|
Osteoporotic bone
|
|
(Figure 1)
|
|
|
| Osteoporosis
Facts…Did you know…? |
|
| • |
Osteoporosis is a major public health threat for more than 28 million Americans. |
| • |
In the U.S. today, 10 million individuals already have the disease and 18 million more have low bone mass, placing them at increased risk for osteoporosis. |
| • |
While women are four times more likely to develop the disease, men also suffer from osteoporosis. |
| • |
8 million American women and 2 million men have osteoporosis, and millions more have low bone density. |
| • |
One out of three women and one in eight men will sustain an osteoporosis-related fracture in their lifetime. |
| • |
10% of African-American women over age 50 have osteoporosis; an additional 30% have low bone density that puts them at risk of developing osteoporosis. |
| • |
While osteoporosis is thought of as an old person's disease, it can strike at any age. |
| • |
Osteoporosis is responsible for more than 1.5 million fractures annually, including: |
|
|
o |
300,000 hip fractures |
 |
|
o |
700,000 vertebral fractures |
|
o |
250,000 wrist fractures |
|
o |
300,000 fractures at other sites. |
|
| • |
The estimated cost for osteoporotic and associated fractures is $13.8 billion ($38 million each day) and the cost is rising. |
| • |
The rate of hip fractures is two to three times higher in women than men; however the one year mortality rate following a hip fracture is nearly twice as high for men as for women. |
| • |
A woman's risk of hip fracture is equal to her combined risk of breast, uterine and ovarian cancer. |
| • |
An average of 24% of hip fracture patients age 50 and over die in the year following their fracture. |
| • |
One-fourth of those who were ambulatory before their hip fracture require long-term care afterward. |
| • |
Women can lose up to 20% of their bone mass in the 5-7 years following menopause, making them more susceptible to osteoporosis. |
| • |
An estimated 26.2 million Americans, of whom 80% are women, are at risk of developing the disease. |
| • |
77% of osteoporotic women are undiagnosed and untreated |
| • |
Early detection and treatment may save as much as 30% to 40% of the current costs, based on research reported by the Endocrine Study. |
|
|
| What are the Risk Factors for Osteoporosis? |
|
| Certain people are more likely to develop osteoporosis than others. Factors that increase the likelihood of developing osteoporosis are called "risk factors." The following risk factors have been identified: |
|
| • |
Being female |
| • |
Thin and /or small framed |
| • |
A family history of osteoporosis |
| • |
Advanced age |
| • |
Postmenopausal, including early or surgically induced menopause |
| • |
Abnormal absence of menstrual periods (amenorrhea) |
| • |
Anorexia nervosa or bulimia |
| • |
A diet low in calcium |
| • |
Use of certain medications, such as corticosteroids and anticonvulsants |
| • |
Low testosterone levels in men |
| • |
An inactive lifestyle with little or no exercise |
| • |
Cigarette smoking |
| • |
Excessive use of alcohol |
| • |
Excessive intake of soda (phosphates) |
| • |
Being Caucasian or Asian (although African Americans and Hispanic Americans are at significant risk also) |
|
|
|
Your Grade Is:
25 to 35 "Yeses" -- Highest Risk
15 to 24 "Yeses" -- High Risk
5 to 14 "Yeses" -- Medium Risk
4 or fewer "Yeses" -- Low Risk
|
|
| This osteoporosis risk questionnaire is a quick way to assess your risk of developing osteoporosis. The more times you answer “yes”, the greater your risk of developing osteoporosis. All information is intended for your general knowledge only and is not a substitute for medical advice or treatment for a specific medical condition. Please consult your physician if you have questions or concerns regarding your risk for osteoporosis. |
|
| Bone Development and Remodeling |
|
| Prior to birth and for several months after birth, the skeleton has very little bone. Many bones start out as cartilage. As the child grows, cartilage transforms into true bone – a process called (endochondral ossification). Ossification rates appear at set times in healthy children and can be evaluated by radiographic imaging or x-rays. Early in life, more bone tissue is added than is taken away. Maximum bone density and strength is reached between ages 25 and 30.
Bones are a storehouse of minerals. They hold 99% of the body’s calcium, 86% of its phosphate, and 54% of our magnesium. Calcium is an essential element in keeping bones healthy and strong. But calcium plays an important role in other essential functions as well:
| • |
Calcium keeps cell membranes permeable |
| • |
Muscles can not contract without calcium |
| • |
Blood can not clot without calcium |
| • |
Certain enzymes can not function without calcium |
|
|
| To keep bones healthy and in good repair, there is a mechanism in place to repair damaged tissue and to revitalize old, weakened bone with new, strong material. Bone is continually maintained through the process of bone remodeling. Bone remodeling has two phases: resorption (removal of old bone) and formation (building of new bone).
The following four steps illustrate the resorption and formation process.
|
|
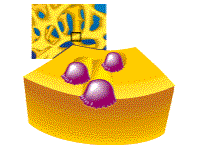 |
Step
1: Specialized cells called osteoclasts attach to and dissolve away existing bone, leaving small indentations on the bone surface. This causes collagen and minerals to be released into the bloodstream. |
|
|
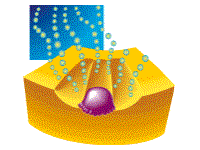
| Step
2: Bone resorption and remodeling begins when hormones are sent out into the bloodstream, triggering osteoclasts to respond to the site where new bone needs to be produced. |
 |
|
|
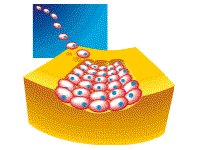 |
Step 3: Once the osteoclasts have prepared the site, osteoblasts move in. “Osteo” means bone and “blast” means to make or form. Osteoblasts converge at the site where bone repair will take place
and proceed to produce a collagen framework. |
|
|
| Step 4: This process results in new bone being formed.
When resorption and formation are in balance, there is no net change in bone mass. |
 |
|
|
| After a resting phase during which the bone is mineralized, the remodeling cycle begins all over again. Approximately 10-20% of our existing bone tissue is replaced annually by this process.
Menopause and Osteoporosis
Menopause is the number one risk factor for osteoporosis in women. Menopause is characterized by a loss of estrogen production by the ovaries. This loss may occur by natural means or by the surgical removal of both ovaries. The loss of estrogens enhances the activity of the osteoclasts (the cells that resorb bone) and decreases the activity of the osteoblasts (the cells that produce bone). The result is a net loss of bone and for many women can lead to osteoporosis. Women can lose up to 20 percent of their bone mass in the 5 to 7 years following menopause.
The condition of an older woman's skeleton depends on two things:
1. The peak amount of bone attained prior to menopause.
2. The rate of bone loss thereafter.
Prevention of Osteoporosis
Osteoporosis is largely preventable for most people. Prevention of this disease is very important because, while there are treatments for osteoporosis, there is currently no cure. Building strong bones, especially before the age of 30, can be the best defense against developing osteoporosis, and a healthy lifestyle can be critically important for keeping bones strong.
There are four steps to preventing osteoporosis. No one step alone is enough to prevent osteoporosis, however, following all four steps may!
| 1. |
Consume a balanced diet rich in calcium, vitamin D and other vitamins and minerals important in maintaining healthy bones
 Calcium plays an important role in maintaining bone. Calcium alone cannot prevent osteoporosis, but it is an important part of an overall prevention or treatment program. Yet, national surveys have shown that many women and young girls consume less than half the amount of calcium recommended to grow and maintain healthy bones. Calcium plays an important role in maintaining bone. Calcium alone cannot prevent osteoporosis, but it is an important part of an overall prevention or treatment program. Yet, national surveys have shown that many women and young girls consume less than half the amount of calcium recommended to grow and maintain healthy bones.
Calcium is needed for the heart, muscles and nerves to function properly and for blood to clot. Inadequate calcium is thought to contribute to the development of osteoporosis. Depending on your age, an appropriate calcium intake falls between 500 and 1500 mg a day: |
|
|
| Population Group |
Recommended Daily Intake |
| Children 1 to 3 years of age |
500 mg |
| Children 4 to 8 years of age |
800 mg |
| Preteens and teens 9 to 18 years of age |
1,500 mg |
| Adults 19 to 50 years |
1,000 mg |
| Adults 51 and older |
1,500** mg |
|
|
|
**NOTE: The National Institutes of Health Consensus Conference and the National Osteoporosis Foundation support a higher calcium intake of 1,500 milligrams per day for postmenopausal women not taking estrogen and adults 65 years or older.
Vitamin D is needed for the body to absorb calcium. Without enough vitamin D, you will be unable to absorb calcium from the foods you eat, and your body will have to take calcium from your bones. Vitamin D comes from two sources: through the skin following direct exposure to sunlight and from the diet. Growing scientific support advocates increased amounts of vitamin D. Experts recommend a daily intake of 800 IU per day. Good food sources of vitamin D are fortified dairy products, egg yolks, saltwater fish and liver.
Vitamin B12 plays an important role in immune function and red blood cell production.
Vitamin C promotes the formation of collagen, which is used in organic bone matrix formation, and aids in the synthesis of structural proteins found in bone. It is an antioxidant that acts to prevent free radical formation and cell damage. Well-known sources of vitamin C are citrus fruits; other sources include deep green leafy vegetables and potatoes.
Vitamin K plays a key role in the synthesis of a key bone protein, osteocalcin. Osteocalcin improves the attachment of bone-resorbing cells to bone and supports bone remodeling. Vitamin K is found in green leafy vegetables (also good calcium sources), and many other foods. Research shows that women who take a sufficient daily amount of vitamin K are less likely to suffer hip fractures.
Folic acid is important for tissue growth and proper cell division and replication. Folic acid works in tandem with vitamins B12 and C in several metabolic processes, including production of blood cells in the bone marrow.
Magnesium is necessary for calcium metabolism into bone and essential in muscle function.
Manganese is a trace mineral needed for healthy bone and cartilage formation.
Zinc is required for proper functioning of enzyme systems in the body and important for tissue renewal and skeletal development. Zinc levels tend to be low in menopausal women.
Copper is part of proteins and enzymes linked with red blood cell function. Plays a role in helping form the connective structures of bones and enhances the effectiveness of vitamin D. Copper levels tend to be low in menopausal women.
Note: If your diet is deficient in calcium or any of the abovementioned nutrients, you should consider taking a daily
supplement. |
|
|
| 2. |
 Participate in regular weight-bearing exercise Participate in regular weight-bearing exercise
Exercise is also important
for bone health. If you exercise regularly in childhood and adolescence, you are more likely to reach your peak bone density than those who are inactive. The best exercise for your bones is weight-bearing exercise such as walking, dancing, jogging, stair-climbing, racquet sports and hiking. Exercise can also be helpful in building and maintaining strong bones. The benefits of exercise last only as long as you maintain the program. Speak with your doctor to learn what type of exercises you can do safely not only to preserve bone, but also to strengthen your back and hips and maintain flexibility. Be sure to check with your healthcare provider before beginning any exercise program. |
|
|
| 3. |
Maintain a healthy lifestyle with no smoking, excessive caffeine intake, or excessive alcohol use

Cigarette smoking was first identified as a risk factor for osteoporosis more than 20 years ago. Subsequent studies have also demonstrated a direct relationship between tobacco use and decreased bone density. Significant bone loss has been found in postmenopausal women with prolonged smoking exposure. In addition, a relationship between cigarette smoking and low bone density in adolescence and early adulthood has been identified. If you smoke, develop a plan now to stop smoking or ask your health care professional to recommend methods to help you quit.
Excessive caffeine from coffee or soda contributes to bone breakdown and may be a factor in the development of osteoporosis.
Excessive alcohol intake interferes with the balance of calcium. It also increases parathyroid hormone (PTH) levels, which in turn reduce the body’s calcium reserves. Calcium balance is further disrupted by alcohol’s ability to interfere with the production of vitamin D, and therefore the absorption of calcium. Cortisol levels tend to be elevated in alcoholics. Cortisol increases osteoclastic bone resorption and accelerates bone loss. Due to the effects of alcohol on balance and gait, alcoholics tend to fall more frequently than non-alcoholics. Heavy alcohol consumption has been linked to an increase in the risk of fracture
including the most serious injury, hip fracture. Vertebral fractures, which tend to be uncommon in individuals under 50 years of age, are more prevalent in those under the age of 50 who abuse alcohol. |
|
|
| 4. |
Have a routine Bone Mineral Density Test
 A Bone Mineral Density test (BMD) is the only way to diagnose osteoporosis and determine your risk for future fracture. Since osteoporosis can develop undetected for decades until a fracture occurs, early diagnosis is important. A BMD test measures the density of your bones (bone mass) and is necessary to determine whether you need medication to help maintain your bone mass, prevent further bone loss and reduce fracture risk. A
BMD test is a special type of test that is accurate, painless and noninvasive. A Bone Mineral Density test (BMD) is the only way to diagnose osteoporosis and determine your risk for future fracture. Since osteoporosis can develop undetected for decades until a fracture occurs, early diagnosis is important. A BMD test measures the density of your bones (bone mass) and is necessary to determine whether you need medication to help maintain your bone mass, prevent further bone loss and reduce fracture risk. A
BMD test is a special type of test that is accurate, painless and noninvasive.
|
|
|
|
ACT NOW AND START YOUR OWN OSTEOPOROSIS PREVENTION PROGRAM!
|
|
| Note: All information on this website is intended for your general knowledge only and is not a
substitute for medical advice or treatment for a specific medical condition. Please consult your
physician if you have questions or concerns regarding your health. |
|
|
|
|
 |

